
Central Disorders of Hypersomnolence
For most people, feeling tired after a poor night’s sleep is a familiar and temporary experience. But for patients with central disorders of hypersomnolence, excessive daytime sleepiness is persistent, overwhelming, and not explained by insufficient sleep the night before. These conditions arise from disruptions within the brain’s own sleep-wake regulatory systems, and they can significantly impair a person’s ability to work, drive, maintain relationships, and function safely in daily life.
At Penn Medicine Becker ENT & Allergy, our experienced ENT doctors recognize that excessive daytime sleepiness is not simply a lifestyle issue or a matter of going to bed earlier. When sleepiness becomes a consistent and impairing presence despite adequate nighttime rest, a thorough evaluation is essential to identify the underlying cause and determine the most appropriate path forward.
What Are Central Disorders of Hypersomnolence?
Central disorders of hypersomnolence are a category of sleep conditions defined by excessive daytime sleepiness (EDS) that cannot be attributed to disturbed or insufficient nocturnal sleep, another sleep disorder, or an underlying medical condition. The word “central” refers to the fact that these disorders originate within the central nervous system’s regulation of alertness, rather than being a consequence of poor or fragmented nighttime sleep.
Patients with these conditions often struggle to remain alert during routine activities such as driving, working, or having a conversation. The sleepiness they experience is not relieved by caffeine or willpower, and it may not fully resolve even after sleeping for extended periods. This distinguishes central hypersomnolence disorders from the fatigue associated with a busy schedule or poor sleep habits.
Types of Central Hypersomnolence Disorders
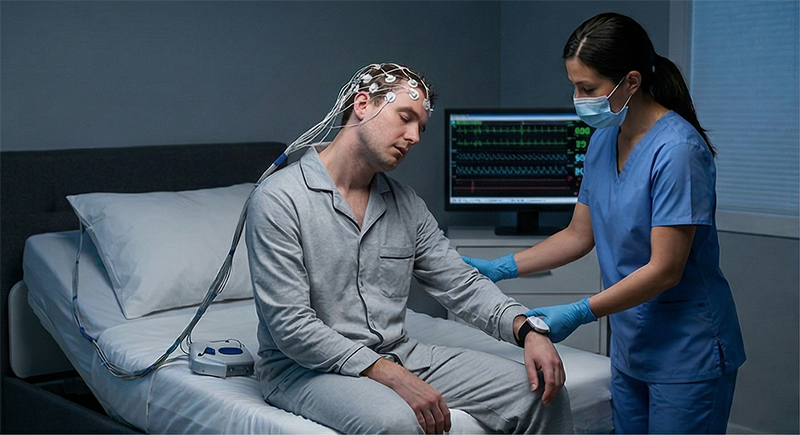
Narcolepsy Type 1
Narcolepsy Type 1 is characterized by two defining features: excessive daytime sleepiness and cataplexy. Cataplexy is a sudden, involuntary loss of muscle tone triggered by strong emotions — most commonly laughter, surprise, or excitement. Episodes can range from mild muscle weakness in the face or limbs to a complete physical collapse, all while the patient remains conscious and aware. Narcolepsy Type 1 is associated with a significant loss of hypocretin (also called orexin), a neuropeptide produced in the hypothalamus that plays a central role in maintaining wakefulness. Additional features may include:
Narcolepsy Type 2
Narcolepsy Type 2 presents with the same pattern of excessive daytime sleepiness seen in Type 1, including intrusive sleep episodes that can occur regardless of how much the patient slept the previous night. The key distinction is the absence of cataplexy.
Hypocretin levels are typically normal or only mildly reduced. The condition still significantly impairs daily functioning and requires a formal sleep evaluation — including overnight polysomnography followed by a Multiple Sleep Latency Test (MSLT) — for accurate diagnosis.

Idiopathic Hypersomnia
Idiopathic hypersomnia is characterized by chronic, excessive sleepiness despite sleeping for long periods — often ten or more hours per night. Unlike narcolepsy, patients do not typically experience cataplexy or sudden sleep attacks, but many describe profound sleep inertia upon waking: a prolonged and disabling difficulty achieving full alertness even after an extended sleep. The term “idiopathic” reflects the fact that no definitive neurological cause has been established, though research into the underlying biology of the condition is ongoing. Idiopathic hypersomnia can be difficult to distinguish from narcolepsy without specialized testing.

Kleine-Levin Syndrome
Kleine-Levin Syndrome is a rare and episodic condition marked by recurring periods of excessive sleep lasting days to weeks, often accompanied by behavioral and cognitive changes. During an episode, patients may sleep 16 to 20 hours per day and exhibit:
Between episodes, patients return to entirely normal functioning with no memory impairment. Episodes can recur multiple times per year and often diminish in frequency over time. The condition most commonly affects adolescent males, though it can occur across demographics. Diagnosis is largely clinical given the rarity of the condition.

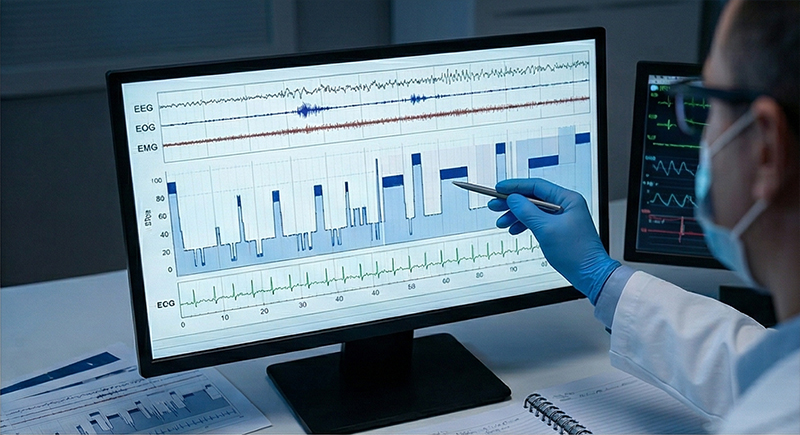
Clinical Variables Measured During a Sleep Study
Diagnosing a central hypersomnolence disorder requires ruling out other causes of excessive daytime sleepiness, including obstructive sleep apnea, insufficient sleep, and circadian rhythm disorders. The following variables are evaluated as part of a comprehensive sleep study:

How Hypersomnolence Disorders Are Diagnosed
The gold standard for diagnosing central hypersomnolence disorders is a two-part sleep study: an overnight polysomnogram followed the next day by a Multiple Sleep Latency Test (MSLT). During the MSLT, patients are given four to five scheduled 20-minute nap opportunities throughout the day. The time it takes to fall asleep during each nap is recorded, as is the presence of REM sleep. A mean sleep latency of eight minutes or less, combined with two or more sleep-onset REM periods, is a key diagnostic indicator for narcolepsy. Idiopathic hypersomnia is characterized by short sleep latency without the REM findings.
Prior to testing, patients are typically asked to maintain a consistent sleep schedule and may be asked to discontinue certain medications that could affect results.

Pick one of our convenient locations
for Central Disorders of Hypersomnolence Care


