
Insomnia Disorders
Sleep is one of the body’s most essential functions, yet for millions of people, it remains frustratingly out of reach. Insomnia disorders are among the most common sleep-related complaints seen in clinical practice, affecting patients of all ages and backgrounds. Characterized by persistent difficulty falling asleep, staying asleep, or waking too early despite having adequate time and opportunity for rest, insomnia can take a serious toll on energy, mood, concentration, and long-term health.
At Penn Medicine Becker ENT & Allergy, our experienced ENT doctors understand that poor sleep rarely has a single, straightforward cause. Whether insomnia is rooted in stress, an underlying medical condition, airway-related sleep disruption, or a combination of factors, we take the time to evaluate each patient thoroughly and work toward a management plan that addresses the full picture.
What Are Insomnia Disorders?
Insomnia disorders are defined not simply by a bad night’s rest, but by a recurring pattern of sleep difficulty that causes measurable distress or impairment in daily functioning. Patients often describe lying awake for long stretches despite feeling tired, waking frequently throughout the night, or rising in the early morning hours without being able to return to sleep. In many cases, the frustration surrounding sleep itself becomes a contributing factor, creating a cycle in which worry about not sleeping makes rest even harder to achieve.
Sleep specialists classify insomnia primarily based on how long it has been present and whether an identifiable trigger can be identified.
Chronic Insomnia
Chronic insomnia is diagnosed when sleep difficulty occurs at least three nights per week and has been present for three months or longer. It is the more clinically significant form of the condition and often requires structured evaluation to identify contributing factors. Chronic insomnia is frequently associated with anxiety, depression, chronic pain, or ongoing medical conditions. In some patients, a phenomenon known as conditioned insomnia develops over time, in which the bedroom environment and bedtime routine become closely associated with wakefulness and distress rather than relaxation and sleep.
Short-Term (Acute) Insomnia
Acute or short-term insomnia is typically tied to a specific, identifiable stressor — a major life event, illness, travel, grief, or a significant change in schedule. Most patients find that their sleep returns to normal once the precipitating circumstance has resolved. However, in some individuals, acute insomnia can transition into a chronic pattern if the initial disruption is not well managed. Recognizing this progression early is an important part of clinical care.

How Sleep Specialists Evaluate Insomnia
When a patient presents with insomnia, the evaluation goes beyond simply asking how many hours of sleep they get. Sleep specialists measure specific variables that help paint an accurate picture of what is happening during the night and how significantly sleep is being disrupted. Three of the most clinically relevant metrics include:

Clinical Variables Measured During a Sleep Study
When a patient enters a sleep lab, our team evaluates a comprehensive set of technical variables to build an accurate diagnostic picture. For insomnia patients, the most relevant include:
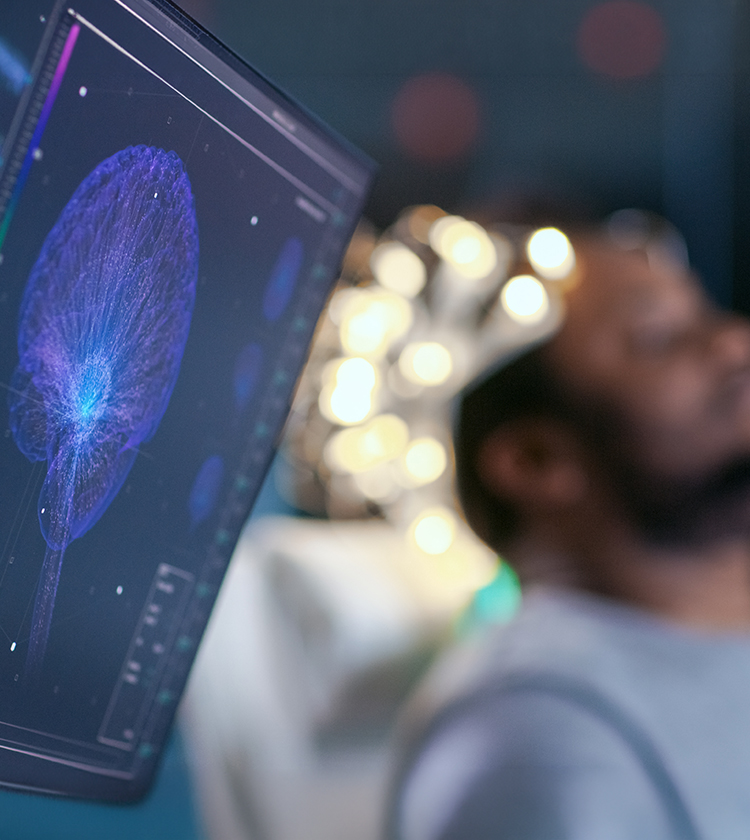


The Relationship Between Insomnia and Airway Health
Insomnia does not always originate from stress or psychological causes alone. In a meaningful number of patients, difficulty sleeping is related to upper airway dysfunction that disrupts sleep continuity without the person being fully aware of it. Conditions such as nasal obstruction, chronic congestion, and sleep-disordered breathing — including Upper Airway Resistance Syndrome (UARS) and obstructive sleep apnea — can cause repeated brief awakenings throughout the night, resulting in the subjective experience of non-restorative or fragmented sleep.
Because Penn Medicine Becker ENT & Allergy specializes in the evaluation and treatment of the upper airway, our team is well positioned to assess whether structural or anatomical factors are contributing to a patient’s insomnia. Treating the underlying airway issue, when one is present, can lead to meaningful improvement in sleep quality.
Contributing Factors to Consider
Insomnia rarely exists in isolation. A variety of behavioral, environmental, and medical factors can play a role, and understanding these contributors is an important part of building an effective management plan.
Sleep hygiene encompasses the habits and environmental conditions that either support or undermine healthy sleep. Relevant factors include irregular sleep and wake schedules, exposure to bright or blue-spectrum light in the evening, room temperature, caffeine intake particularly in the afternoon and evening, alcohol use, and the use of electronic devices before bed. While addressing sleep hygiene alone may not resolve all cases of insomnia, it is frequently an important foundational step.
Medical contributors to insomnia are wide-ranging and include chronic pain conditions, gastroesophageal reflux, thyroid disorders, anxiety, and depression. Certain medications can also interfere with sleep architecture or sleep onset. A comprehensive evaluation considers all of these possibilities and helps prioritize which contributors most warrant attention.
When to Seek Evaluation
Patients are encouraged to seek evaluation when sleep difficulty has been present for several weeks or longer, when it is occurring on most nights of the week, or when poor sleep is affecting their ability to function during the day. Early evaluation is particularly valuable because it can identify underlying factors — including those related to the airway — that can be addressed before a short-term problem becomes chronic.

Pick one of our convenient locations
for your Insomnia Disorder Treatment


