Meet Bradykinin – it’s a natural substance in our bodies that helps control things like blood pressure and inflammation. But for some people, who are affected by a genetic condition known as hereditary angioedema (HAE), it can become a problem. Their bodies can’t regulate bradykinin properly, causing parts of their body to swell up unexpectedly. Everywhere from the arms and legs to the face and even the airways can be affected. Now, scientists are looking to bradykinin as the key to both understanding and treating this disorder. Step by step, they’re unraveling the complex secrets of this unique peptide and its role in our body.
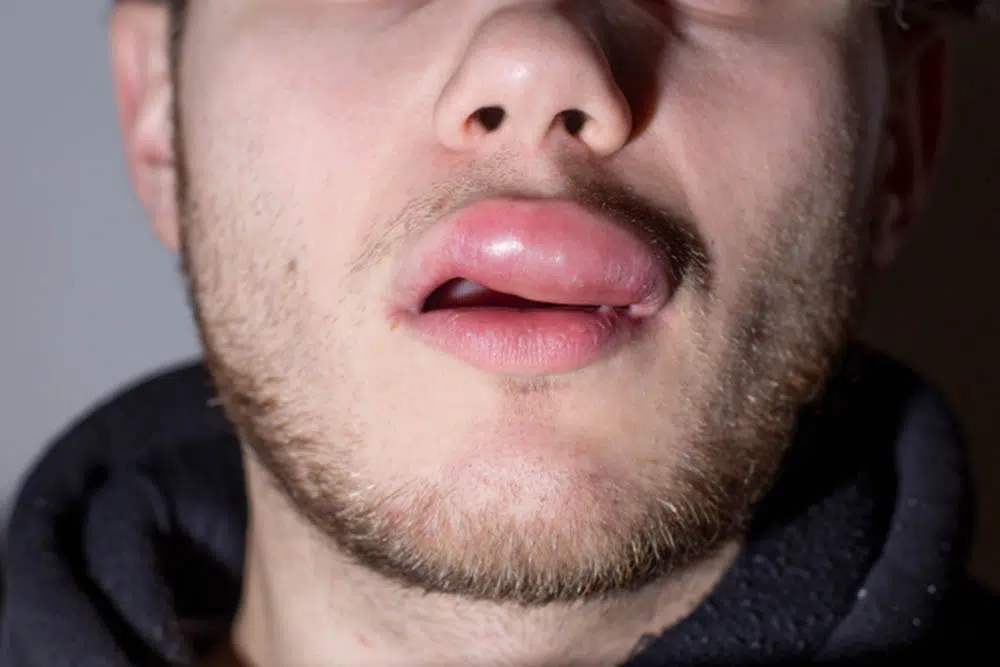
Understanding Bradykinin in Relation to Hereditary Angioedema
Bradykinin, a peptide that dilates blood vessels and makes them more permeable, plays a substantial role in hereditary angioedema. This disorder, passed down through families, is characterized by swelling or angioedema in adults and children. With this condition, faulty regulation of bradykinin causes the body’s blood vessels to leak and leads to sudden swelling attacks. The concern is that these attacks can affect various areas of the body, including the intestines, arms, legs, face, and even the airways.
Due to the inherent genetic factor in HAE, some individuals naturally produce more bradykinin than others. This excessive production manifests as repeated episodes of swelling in different parts of the body. Exactly where the attacks occur and how severe they are, can be significantly influenced by the amount of bradykinin present in the system at any given moment.
Bradykinin isn’t naturally harmful, but in the case of people with HAE, the regulation of this substance becomes dysfunctional. It causes a loss of control over blood vessel permeability, leading to angioedema in adults and children. Treatments typically focus on reducing the body’s production and release of bradykinin, thus curbing the intense swelling.
While clinical studies continue to investigate how bradykinin and HAE interact, reducing the body’s production of this peptide remains the primary goal. Early diagnosis and managing the condition through treatment are essential to living with the disease.
Intricacies of Bradykinin
Bradykinin, a well-recognized peptide, is quite renowned for its intriguing structure. We owe many biological effects to this wonder molecule, including inflammation. The effects of bradykinin are a result of bradykinin binding to kinin receptors, including B2 receptors.
Interestingly, the biological effects are not a one-time deal. They depend on the degradation of bradykinin. When bradykinin degrades quickly, there is less inflammation. But if the slightest signal delays this degradation, it drastically increases inflammation test results.
The effects on B2 receptors are equally crucial in this process. When bradykinin binds to these receptors, it could lead to various internal changes. Hence, frequent interactions between bradykinin and the B2 receptors can affect the organism’s overall functionality.
To accomplish an effective degradation of bradykinin, the organism employs various enzymes. These enzymes cleave the peptide, significantly reducing the prevalence of the so-called biological effects. Failure in this process could once again result in an amplified inflammation.
In hindsight, the functionality of bradykinin, be it through B2 receptors interplay or through influencing inflammation, stems from its structure. It is these intricate details about bradykinin that make it an extensive field of study.
Bradykinin Structure
- A peptide that causes dilation of blood vessels.
- Consists of nine amino acids.
Functionality
- Initiates inflammation.
- Binds to B2 receptors.
- Degraded by enzymes to limit biological effects.
Biological Effects
- Dilation and contraction of blood vessels.
- Initiates inflammation.
- Can influence pain and blood pressure.
Impact of Bradykinin Antagonists in Patients with Hereditary Angioedema
Bradykinin antagonists offer a reprieve to patients with HAE. The therapeutic interventions include the use of bradykinin antagonists. Bradykinin B2 receptor antagonist works by blocking the effects of bradykinin, which as we mentioned before, is a peptide that causes blood vessels to dilate and, consequently, leads to swelling.
Another application of bradykinin antagonists in the treatment of HAE comes in alleviating recurring attacks. Patients grappling with frequent bouts of swellings have found relief by using bradykinin antagonists. The therapeutic interventions offered are not just geared towards managing episodes but also preventing them.
Contrary to other treatments, the use of bradykinin B2 receptor antagonists offers minimized side effects. With fewer adverse effects seen in patients, bradykinin antagonists have proven to be a plausible alternative. Studies indicate positive responses among patients who have incorporated the antagonists as part of their treatment plan.
The advent of bradykinin antagonists has brought forth a leap in the management of HAE. With the application of antagonists, patients have experienced a reduction in the severity and frequency of swelling episodes. This impactful approach has created a clinical shift in managing the condition.
Nevertheless, continual studies are needed for the exploration of more effective ways of using bradykinin antagonists. However, the current data point towards a promising future in the quest to offer quality care to patients with HAE.
Management of Acute Angioedema Attacks in Adults Using Bradykinin Antagonists
In the battle against acute angioedema attacks in adults, we are leveraging the power of bradykinin B2 receptor antagonists. These attacks in adults can lead to severe inflammation and discomfort. Bradykinin is a potent inflammatory mediator, heightening the body’s reaction during an angioedema attack.
Used effectively, bradykinin antagonists can significantly alleviate symptoms. We ensure better management of acute attacks by blocking the effects of bradykinin. Working via this method reduces the inflammation and swelling that characterizes an acute angioedema attack.
Another pivotal use of bradykinin B2 receptor antagonist is in patients with hereditary angioedema. HAE is a genetic disorder leading to recurrent episodes of severe swelling. By blocking bradykinin, patients with this disorder can live normally without the fear of sudden acute attacks.
Bradykinin antagonists have been important tools in managing conditions related to angiotensin-converting enzymes (ACE). Often, patients react adversely to ACE inhibitors, leading to angioedema. By using bradykinin antagonists, we counteract these adverse responses, providing relief to patients.
However, like any medication, bradykinin antagonists also have side effects. Patients may experience changes in heart rate, and blood pressure, or develop a cough. We constantly evaluate its effectiveness to ensure its benefits outweigh the potential side effects.
Overall, bradykinin antagonists have revolutionized the management of acute angioedema attacks. By curbing the inflammation and swelling associated with attacks, these drugs provide relief to patients. Furthermore, its use in managing HAE suggests promising possibilities for future treatments.
Types of Bradykinin Antagonists Used in HAE
Icatibant
Icatibant is a peptide antagonist that functions by directly blocking the bradykinin B2 receptor. This synthetic decapeptide mimics the structure of bradykinin but does not activate the receptor, effectively preventing bradykinin from exerting its effects on the vascular system.
It is particularly effective in treating acute attacks of HAE, with the ability to be administered subcutaneously by patients themselves. Its rapid onset of action typically brings symptom relief within hours.
Ecallantide
Ecallantide works by inhibiting plasma kallikrein, an enzyme responsible for cleaving high-molecular-weight kininogen to release bradykinin. By preventing the synthesis of bradykinin, ecallantide reduces its pathological actions during HAE attacks.
It is approved for use in acute HAE attacks and is administered via subcutaneous injection. The medication can be provided in a healthcare setting by a medical professional, given its potential for anaphylactic reactions.
Lanadelumab
Lanadelumab is a monoclonal antibody that binds to plasma kallikrein and inhibits its activity. Targeting kallikrein also reduces the production of bradykinin.
This drug is used as a prophylactic treatment to prevent HAE attacks. Given its longer half-life, lanadelumab is administered every two to four weeks, providing prolonged protection against HAE episodes.
Each of these bradykinin antagonists offers a unique approach to managing HAE, allowing for tailored treatment plans based on the severity and frequency of a patient’s episodes, as well as their individual response to therapy.
Benefits of Bradykinin Antagonist Therapy
Reduction in Frequency of HAE Attacks
Bradykinin antagonist therapy has demonstrated a notable decrease in the frequency of HAE attacks. By inhibiting bradykinin type 2 receptors, these therapies directly mitigate the increase of bradykinin levels typically responsible for episodes of angioedema. The genetic mutation affecting plasma proteins involved in bradykinin generation becomes less impactful as these antagonists curb the overproduction of bradykinin, thereby reducing the frequency and severity of attacks.
Improvement in Quality of Life for HAE Patients
Beyond reducing attack frequency, bradykinin antagonist therapy enhances the overall quality of life for patients. By controlling acute attacks and the vascular remodeling associated with chronic HAE, these treatments allow individuals to participate more fully in daily activities. Pediatric patients, particularly, benefit from this as it contributes to more normal growth and development patterns.
In conclusion, the advent of bradykinin receptor antagonists has been revolutionary in managing hereditary angioedema. These drugs’ inhibitory activity on the bradykinin pathway has not only reduced the incidence of acute HAE episodes but also offered beneficial effects in terms of limiting the progressive aspect of vascular remodeling. While attention to potential drug interactions and adverse reactions remains paramount, the prognosis for HAE patients has significantly improved.
The therapeutic use of bradykinin antagonists, particularly the antagonist of bradykinin B2 receptors, has mitigated the biological effects of unregulated bradykinin production due to gene mutation. These advancements have provided a substantial leap forward in addressing the complex interplay of extracellular signals in HAE. The common side effects are a consideration, and the impact on special populations, such as pregnant women, requires ongoing research. Nevertheless, the therapy’s capacity to improve the frequency and severity of attacks in patients marks a pivotal step in HAE management.
If you or a loved one are suffering from the symptoms of hereditary angioedema, contact Becker ENT and Allergy today to learn more about the revolutionary bradykinin antagonist therapies that can help reduce the frequency and severity of attacks. Let Becker ENT and Allergy’s experienced team provide you with the information you need to make an informed decision when it comes to managing your condition.

